![[HERO] Why iPSC-Derived Cell Therapy is the](https://cdn.marblism.com/zwoaZB6DGse.webp)
For medical oncologists navigating the landscape of cellular immunotherapy, the conversation around cancer relapse has shifted from if to when: and more importantly, how often we can intervene. While autologous CAR-T therapies have demonstrated remarkable initial response rates in hematologic malignancies, the durability question remains unresolved. iPSC-derived cell therapy represents a fundamental departure from this single-shot paradigm, offering what might be best described as an immunological “subscription model” for cancer surveillance and control.
The Autologous Ceiling: Why Current Therapies Hit a Wall
The architecture of contemporary CAR-T therapy contains an inherent constraint: it is biologically finite. Each patient’s T cells must be harvested, engineered, expanded, and reinfused: a process that typically yields a single therapeutic dose. When relapse occurs, clinicians face a stark reality: the original cell source may be depleted, dysfunctional, or simply unavailable for re-manufacturing.
This limitation becomes clinically significant when considering that relapse rates in solid tumors remain stubbornly high, even with initial CAR-T response. The challenge isn’t simply achieving tumor clearance; it’s maintaining immunological pressure over months and years as residual disease attempts to re-establish itself.

Infinite Sourcing: The iPSC Advantage
iPSC-derived cell therapy fundamentally rewrites this equation by decoupling therapeutic cells from individual patient biology. A single healthy donor’s cells can be reprogrammed into induced pluripotent stem cells, then differentiated into therapeutic effector populations: T cells, NK cells, or hybrid lineages: in theoretically unlimited quantities.
This isn’t merely a manufacturing convenience. It enables cancer relapse prevention strategies that were previously impossible: repeated dosing at predetermined intervals, dose escalation based on minimal residual disease monitoring, and combination scheduling with other modalities without the constraint of cell availability.
The clinical implications are immediate. Where autologous therapy forces a binary decision: use the available cells now or lose the option: allogeneic iPSC-derived products allow oncologists to design longitudinal treatment protocols that adapt to disease dynamics rather than manufacturing limitations.
Persistence Redefined: CIML NK Cells and Memory Enhancement
The concept of immunological memory has traditionally belonged to T cell biology, but recent advances in immunological memory oncology have demonstrated that NK cells can also be “trained” for enhanced persistence and recall responses. Cytokine-induced memory-like (CIML) NK cells, generated through exposure to IL-12, IL-15, and IL-18, exhibit heightened cytotoxicity and interferon-γ production that persists weeks after initial activation.
When this memory-enhancing approach is applied to iPSC-derived NK cells, the result is a therapeutic product with both off-the-shelf availability and extended functional durability. In preclinical models of ovarian cancer, these enhanced NK cells have demonstrated sustained antitumor activity through multiple dosing cycles: a critical proof of concept for the “long game” strategy.
The Off-the-Shelf Revolution
FT500 and similar next-generation immunotherapy products represent the first wave of truly off-the-shelf cellular therapies. Unlike autologous manufacturing, which requires weeks of patient-specific processing, these allogeneic products can be thawed and administered within hours of clinical decision-making.
This logistical shift has profound clinical implications beyond convenience. It enables:
Immediate intervention at relapse detection: When minimal residual disease is identified through ctDNA monitoring or imaging, treatment can begin immediately rather than after a 3-4 week manufacturing delay.
Outpatient dosing schedules: Repeated administrations become feasible in ambulatory settings, reducing hospitalization requirements and improving quality of life.
Combination timing optimization: Oncologists can precisely coordinate cellular therapy with radiation, chemotherapy, or checkpoint inhibition without being constrained by manufacturing lead times.
Genetic Engineering at Scale
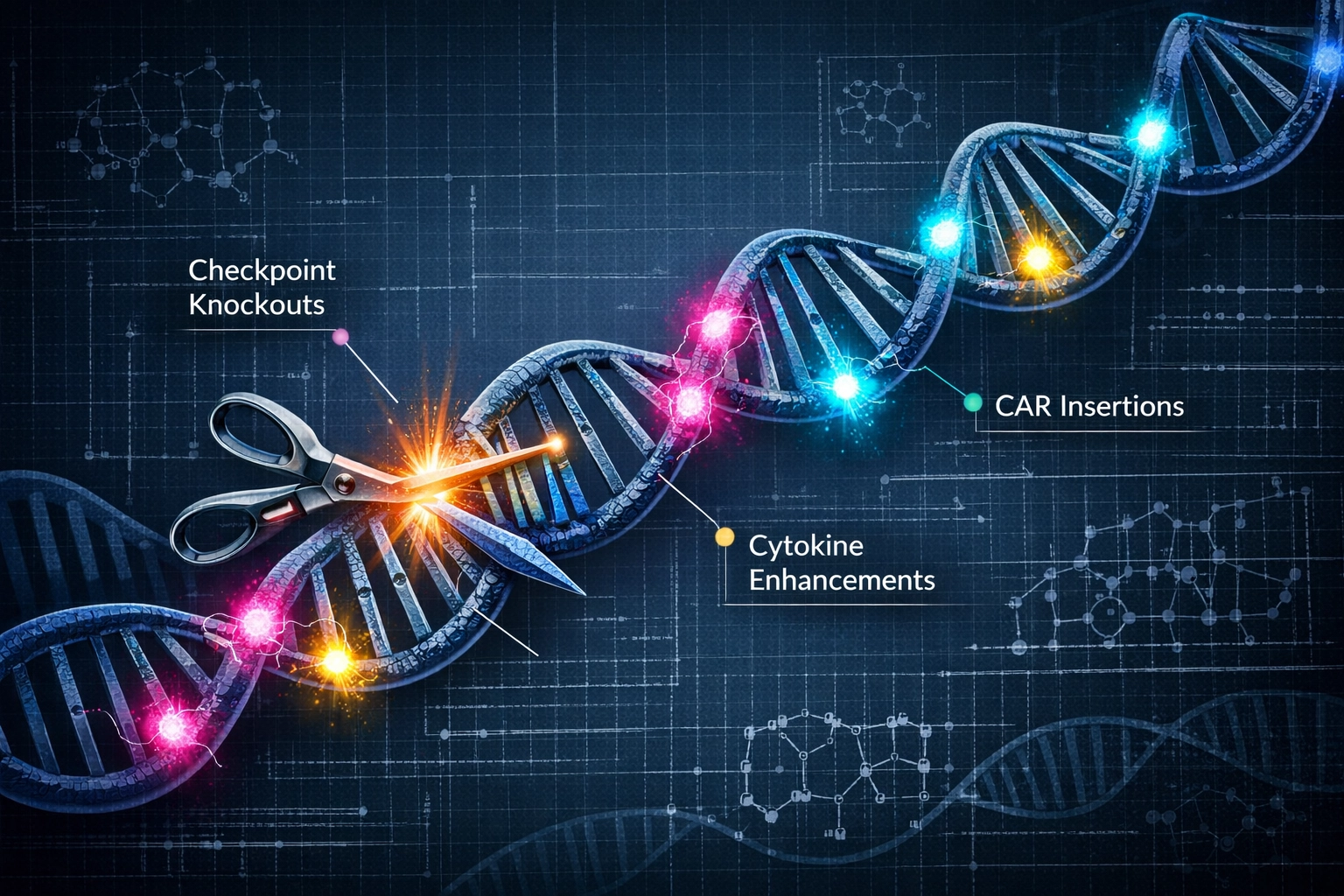
The iPSC platform offers something that autologous therapy cannot: the ability to incorporate genetic modifications at the master cell bank level, ensuring every therapeutic dose contains identical enhancements. Targeted knockouts of immune checkpoint genes: PDCD1 (PD-1), LAG3, CTLA4: can be introduced once and then propagated across millions of doses.
This standardization matters clinically because it eliminates patient-to-patient variability in engineered cell function. When relapse occurs and retreatment is necessary, clinicians can be confident that the second, third, or fourth dose contains the same functional capabilities as the first.
Moreover, the iPSC approach enables multiplexed engineering strategies that would be prohibitively complex in autologous settings. Cells can simultaneously express tumor-targeting CARs, resist checkpoint-mediated exhaustion, secrete immunostimulatory cytokines, and display enhanced trafficking markers: all while maintaining stable expression across cellular generations.

Combination Architecture: Building Synergistic Protocols
The “long game” for cancer relapse prevention increasingly involves not just cellular therapy alone, but strategically designed combinations that exploit complementary mechanisms. iPSC-derived cells serve as an ideal platform for such approaches because their availability enables flexible scheduling around other modalities.
Radiotherapy, for instance, can induce immunogenic cell death and upregulate NKG2D ligands on tumor cells: precisely when subsequent iPSC-NK cell dosing would be most effective. Rather than hoping that a single autologous CAR-T infusion coincides with optimal tumor immunogenicity, clinicians can time repeated allogeneic doses to capitalize on radiation-induced sensitization.
Similarly, checkpoint inhibitors can be administered to remove suppressive signals from the tumor microenvironment just as fresh iPSC-derived effector cells are introduced. This temporal coordination, impossible with single-dose autologous therapy, may explain why early combination trials are showing response rates that exceed either modality alone.
Clinical Implementation: From Theory to Practice
For medical oncologists considering how iPSC-derived cell therapy might integrate into practice, several implementation models are emerging:
Maintenance dosing protocols: Following initial tumor reduction with conventional therapy, patients receive quarterly or biannual iPSC-cell infusions as relapse prophylaxis: analogous to maintenance rituximab in lymphoma but with a cellular mechanism.
Adaptive intensity regimens: ctDNA monitoring guides dosing frequency, with increased administration intervals when molecular relapse is detected and spacing when deep molecular responses are maintained.
Bridge-to-transplant applications: iPSC-cells maintain disease control in transplant-eligible patients during the often-prolonged waiting period for donor matching and conditioning.
The safety profile of allogeneic iPSC products requires careful consideration, particularly regarding graft-versus-host disease (GVHD) risk. However, early clinical data from iPSC-NK therapies have shown minimal GVHD incidence, likely due to NK cells’ reduced alloreactivity compared to T cells and the incorporation of safety switches that enable rapid cell elimination if toxicity emerges.
The Relapse Prevention Paradigm
Traditional oncology has operated on an eliminate-and-observe model: achieve complete remission, then monitor for recurrence. Next-generation immunotherapy using iPSC-derived cells suggests an alternative: achieve remission, then maintain continuous immunological surveillance through repeated cellular dosing.
This paradigm shift aligns with emerging data showing that micrometastatic disease persists in many patients who appear to be in complete remission. Rather than waiting for this minimal residual disease to expand into clinical relapse, repeated immunological pressure could suppress emergence indefinitely: or at least extend progression-free intervals substantially.
Future Directions: What’s on the Horizon
The field of immunological memory oncology continues to evolve rapidly. Current research directions include:
Memory T cell differentiation protocols: Moving beyond effector cells to generate iPSC-derived central memory and stem cell memory T cell phenotypes with enhanced self-renewal capacity.
Tissue-resident memory populations: Engineering iPSC cells to home to and persist in specific tumor microenvironments, creating localized immunological “checkpoints” that prevent metastatic seeding.
Smart cells with biosensor circuits: Incorporating synthetic biology circuits that enable iPSC-cells to respond autonomously to tumor antigens or microenvironmental signals, reducing the need for clinician-directed dosing.
Strategic Considerations for Oncology Practice
As iPSC-derived cellular therapies move through clinical development, several strategic questions warrant consideration:
How will insurance coverage evolve for repeated-dose cellular therapy protocols? Current reimbursement models are designed around one-time CAR-T administration, not longitudinal cellular maintenance.
What patient selection criteria will optimize outcomes? Early data suggest that patients with lower tumor burden and less immunosuppressive microenvironments respond best: but the ability to redose may change these predictive factors.
How should minimal residual disease monitoring be integrated? The availability of repeated dosing makes MRD-directed treatment intensification feasible, but optimal MRD thresholds and monitoring frequencies remain to be determined.
The Long Game in Context
Ultimately, iPSC-derived cell therapy represents more than a manufacturing innovation. It’s a conceptual shift from immunotherapy as a single intervention to immunotherapy as an ongoing process: from hitting cancer hard once to maintaining persistent pressure over time.
For the medical oncologists treating patients who face high relapse risk, this shift offers something that has been frustratingly elusive in solid tumor immunotherapy: options. When relapse occurs, there’s a next move. When minimal residual disease is detected, there’s an intervention that doesn’t require waiting weeks for manufacturing. When initial response is achieved, there’s a strategy for maintaining it.
The “long game” isn’t just about persistence of individual cells: though that matters. It’s about persistence of therapeutic options, persistence of clinical strategy, and ultimately, persistence of hope for patients navigating the complex landscape of cancer treatment and recurrence.
For more information about how Immumem Therapeutics is advancing memory-based cellular immunotherapy, visit our science page or explore our current pipeline.